Health News
29 seconds ago
Amazon shoppers dub this the ‘most flattering T-shirt ever’ — get it for under $20
While your dresser is probably chock-full of T-shirts, do you ever feel like they’re just a little … meh? Sure, you can dress up a plain tee, but unless you want to pile on the accessories, a…
Health News
8 hours ago
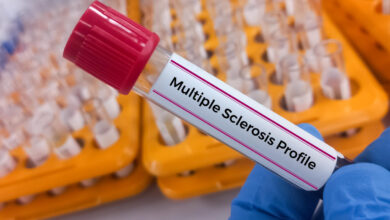
Signs of multiple sclerosis can be detected in blood 5 years before symptoms appear, new study finds. Here’s why this breakthrough is important.
A new study found that in about 10% cases of multiple sclerosis, the body begins producing a distinctive set of antibodies against its own proteins years before symptoms emerge. “Multiple sclerosis is a complex autoimmune disease that…
Health News
20 hours ago
25% of U.S. adults say they drink 1 or 2 glasses of water a day — and 8% rarely or never drink it, Yahoo/YouGov poll finds. Here’s how to sneak more hydration into your day.
A new Yahoo News/YouGov poll has revealed that many Americans are coming up short in hydration. The survey of 1,746 U.S. adults, conducted from April 11 to April 15, found that 8% say they rarely or never…
Health News
1 day ago
Olivia Munn is going through medically induced menopause after breast cancer treatment. Here’s what that means.
Olivia Munn is in medically induced menopause as a result of treatment to keep her breast cancer from recurring, the actress told People in an exclusive new interview. Munn, who last month revealed she’d undergone a double…
Health News
2 days ago
Wanna flex your green thumb this season? According to a professional gardener, you should have these 11 tools on hand
I write about home and kitchen products for a living, so if you’re looking for a new vacuum or air fryer, I’m your gal. But I’ll be the first to admit that when it comes to gardening,…